Our Story
Garran Medical Imaging is a state of the art medical imaging centre in Canberra, Australia. The centre was established in 2015. This centre was an idea that grew from a desire to make a difference. Its founders (Iain Duncan, Kevin Osborn, and Nick Ingold) were not prepared to be complacent, to accept the status quo, or to keep doing things the same way. Over years in medical imaging they all developed a desire, an idea, a hunger to do things better. The entire team at Garran Medical Imaging share this passion.
We are a small team that really tries to make a difference. Garran Medical Imaging aims to be an integral part of the healthcare solution for both patients and their doctors.
The patient journey, from referral through booking, check–in, the scanning procedure, the analysis and reporting, and the delivery of results, is carefully mapped to ensure a comfortable, productive and stress-free experience. Our equipment and staff are able to provide state of the art imaging by adopting the best techniques available and adapting them for the specific needs of our referral patterns.
Our hybrid imaging is done without compromise – see this 1-minute video on xSPECT molecular imaging.
5 Questions to
Dr. Iain Duncan
 How does the centre work with hybrid imaging?
How does the centre work with hybrid imaging?
Our centre has a strong musculoskeletal bias and the hybrid imaging is used mostly in the context of assessing complex musculoskeletal cases. We use xSPECT/CT and direct quantification often in combination with either MRI or ultrasound. I started my career as a rheumatologist, so I often combine imaging and clinical evaluation to optimise the use of imaging to assess difficult diagnostic and management problems. We have established a large database of xSPECT/CT and xSPECT Quant cases and are currently developing the use of direct quantification in musculoskeletal and oncology diagnosis. In 2017 we have added Tc-PSMA imaging to our stable (tracer from Tecnology University of Munich). Currently we are the only site in Australia offering this service and our experience to date is very positive.
What is the newest instrument in your program? Why did you choose that one in particular?
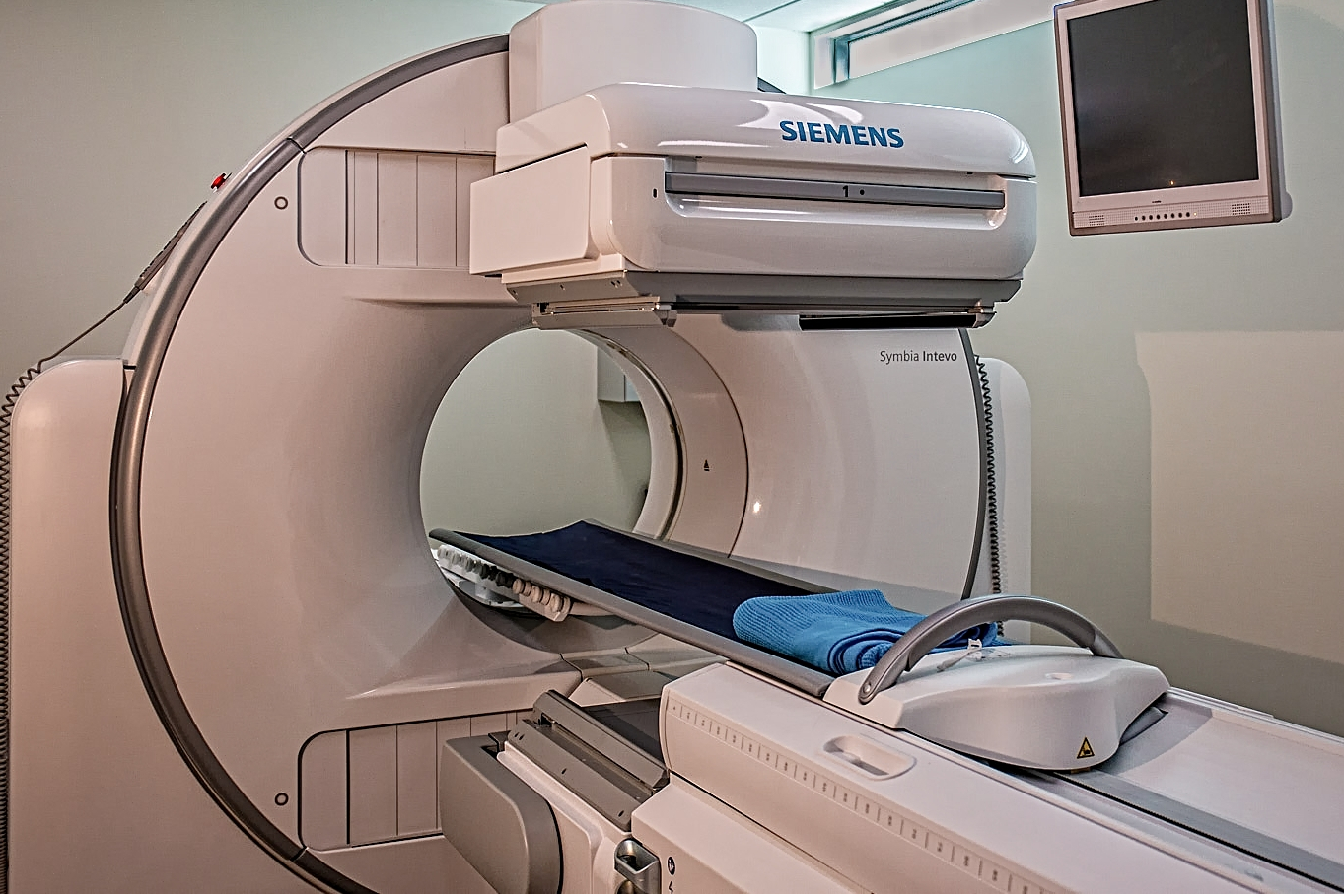
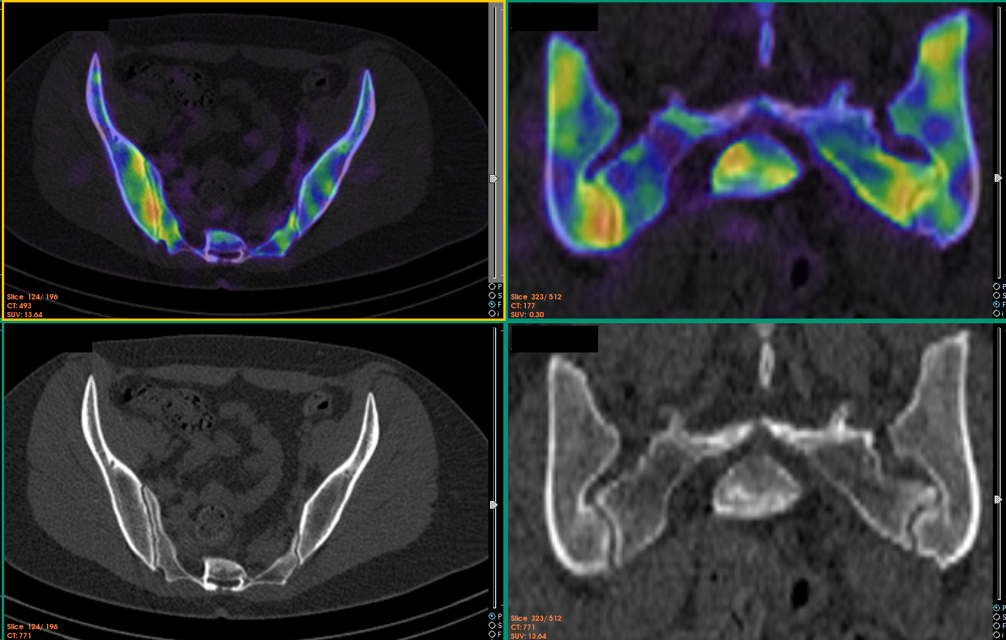
When we opened the centre in 2015 we acquired an Intevo xSPECT/CT from Siemens and in addition opted to use the new xSPECT/CT bone reconstruction. Later we added direct quantification. We believe this is currently the best hybrid gamma camera solution. Both our onsite technical testing and our subsequent experience support this choice. We undertook a prospective evaluation after installing the equipment -that is currently in press (European Journal of Hybrid Imaging). The addition of quantification has added a whole new level of accuracy to serial assessment of oncology cases –both for Bone and PSMA studies. The higher resolution of xSPECT is particularly important with Tc-PSMA, where the SPECT resolution becomes much closer to gallium PET PSMA. It then becomes improtant to consider the resolution of the CT scan, as in soft tissue hybrid imaging it is the lower resolution CT that can limit the system sensitivity (eg size of lymph nodes in Tc-PSMA scans).
Quantification is also proving useful in Tc-pyrophosphate scans for cardiac amyloid.
How do the benefits outweigh the costs?
This is a difficult question to be objective about. Unquestionably we believe our hybrid imaging has provided much better patient assessment. I report hybrid imaging scans from a number of other centres and it is clear that older and cheaper systems cannot provide the level of anatomic sensitivity and specificity of our system. We do not charge any more for these more expensive solutions, so ultimately the stand-alone business case for better quality is not strong -we rely on being able to attract more referrals to our centre. Ultimately, we do it because we care about our patients.
How do Radiologists and Nuclear Medicine Physicians collaborate at your medical center?
I work closely with Dr Kevin Osborn our radiologist. We share a reporting office which is literally at the centre of our practice. This allows us to have frequent dialogue on an hour to hour basis. Kevin specialises in MRI but we both do ultrasound and I have a strong understanding of bone CT as a result of many years in hybrid imaging. We can discuss patients who have had both hybrid imaging and MRI for example. If required we can do software fusion of MRI and SPECT/CT, though in practice this is rarely required. We also understand the strengths and weakness of all of the available imaging modalities. For example we can immediately discuss the appropriateness of an MRI versus a bone scan in a patient that we are having diagnostic difficulty with using ultrasound. Having previously spent some time in a facility that did only ultrasound and hybrid imaging I can highly recommend the benefits of radiology and nuclear physicians working side by side.
What will the future hold for hybrid imaging?
I am optimistic, as it is clear that over the last 10 years in general nuclear medicine the resolution of systems has improved enormously, both following the introduction of hybrid imaging and with the improvement of those systems. It is clear that hybrid imaging can provide a more accurate and useful assessment than pure anatomic imaging. PSMA and bone imaging are both great examples of this. As more tracers are developed the clinical utility of hybrid imaging can only improve. Direct Quantification will also become a more integral part of SPECT hybrid imaging, most particularly in oncology.
Dr. Iain Duncan
|
Dr. Duncan’sCase to Remeber
|
More Stories
ESHI Story No. 8
Misr Radiology Center
(Cairo, Egypt)
ESHI Story No.7 (Video)
PETSCAN Vienna
(Vienna, Austria)
ESHI Story No. 6 (Video)
Nuclear Medicine Department / Hospital Sant Pau
Barcelona, Spain
Would you like to publish your centre on our website and share your story with our community?
Contact: office@eshi-societ.org